The study, published today in Cell Stem Cell, shows that it is possible to experiment on a developing human placenta, rather than merely observe specimens, in order to study major disorders of pregnancy.
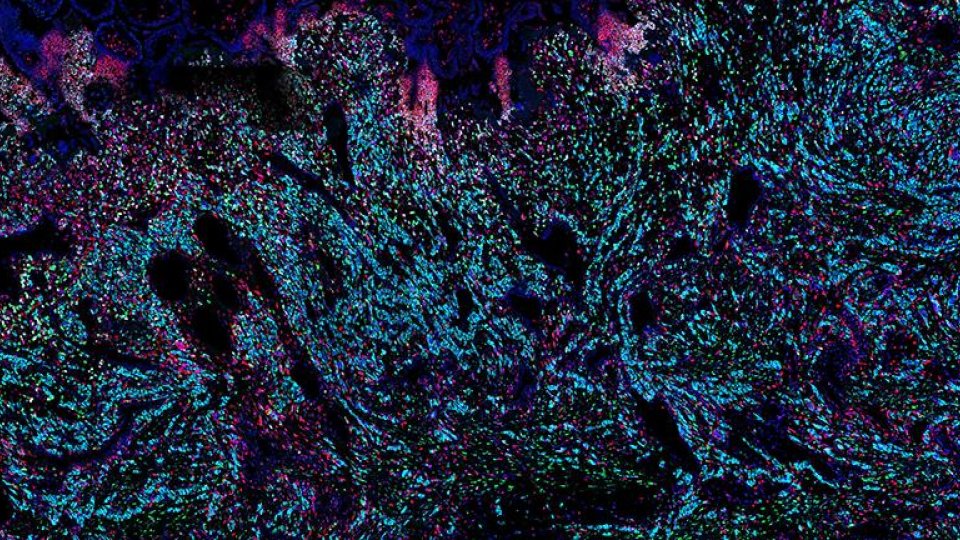
Successful pregnancy depends on the development of the placenta in the first few weeks of gestation. During this period, the placenta implants itself into the endometrium – the mucosal lining of the mother’s uterus. Interactions between the cells of the endometrium and the cells of the placenta are critical to whether a pregnancy is successful. In particular, these interactions are essential to increase the maternal blood supply to the placenta, necessary for fetal growth and development. When these interactions do not work properly, they can lead to complications, such as pre-eclampsia, a condition that causes high blood pressure during pregnancy. Pre-eclampsia occurs in around six in 100 first pregnancies and can put at risk the health of both the mother and the baby.
King's Fellow Ashley Moffett said:
Most of the major disorders of pregnancy – pre-eclampsia, still birth, growth restriction, for example – depend on failings in the way the placenta develops in the first few weeks. This is a process that is incredibly difficult to study – the period after implantation, when the placenta embeds itself into the endometrium, is often described as a ‘black box of human development’.
Over the past few years, many scientists – including several at Cambridge – have developed embryo-like models to help us understand early pre-implantation development. But further development is impeded because we understand so little about the interactions between the placenta and the uterus.
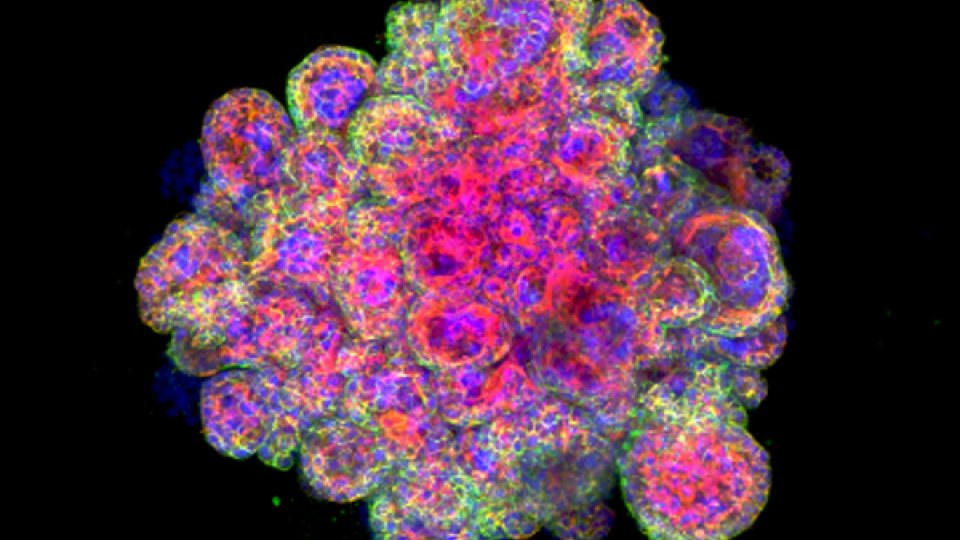
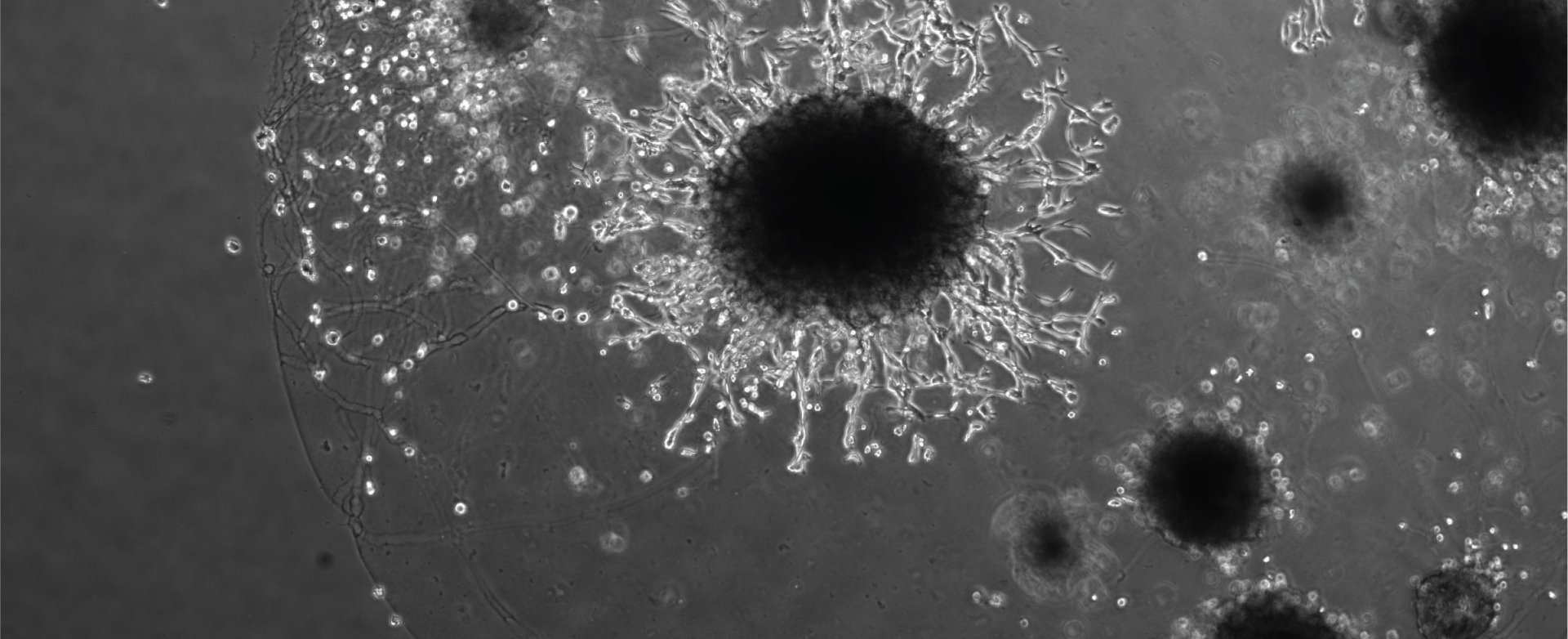
Professor Moffett and colleagues at the Friedrich Miescher Institute, Switzerland, and the Wellcome Sanger Institute, Cambridge, have used ‘mini-placentas’ – a cellular model of the early stages of the placenta – to provide a window into early pregnancy and help improve our understanding of reproductive disorders. Known as ‘trophoblast organoids’, these are grown from placenta cells and model the early placenta so closely that they have previously been shown to record a positive response on an over-the-counter pregnancy test.
The research was supported by Wellcome, the Royal Society, European Research Council and Medical Research Council.
You can read more about this study here.